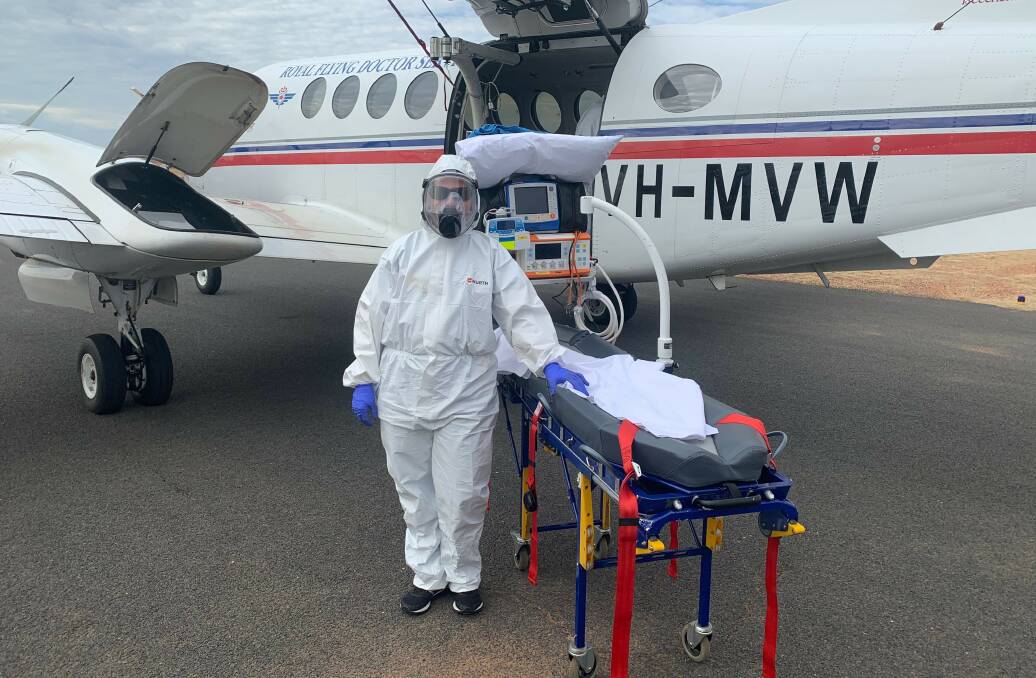
Royal Flying Doctor Service nurse Lydia Newton remembers the time she held the hand of an elderly female patient for three hours while flying her for treatment.
Subscribe now for unlimited access.
$0/
(min cost $0)
or signup to continue reading
"That's a long time to hold hands, not the most comfortable position, " Lydia says.
"I could tell she needed someone to listen to her fears. Older patients often face many unknowns and they worry a lot about their animals they've left behind and are fearful of what procedures or diagnosis they may find in hospital."
But the reassuring hand has been a lot harder to give in the age of coronavirus with social distancing and sometimes with flights now on full COVID-19 alert with cabin crew in full Personal Protection Equipment (PPE).
Lydia has been a registered nurse for 17 years and an RFDS nurse for four-and-a-half years and has flown all over the state with patients to remote towns such as Wilcannia and Lightning Ridge in far western NSW.
The latter is a hotspot for RFDS transfers as often grey nomads on their way to Queensland sometimes need emergency care.
It's a job Lydia loves and she says she gets invaluable support from her colleagues, but the pressure of being COVID-19 wary has been stressful, not only for her, but also for her immediate family in Dubbo, in NSW's Central West, her two children, and her husband who is classed as an essential worker as a postie, and for her older mother who lives on their property.
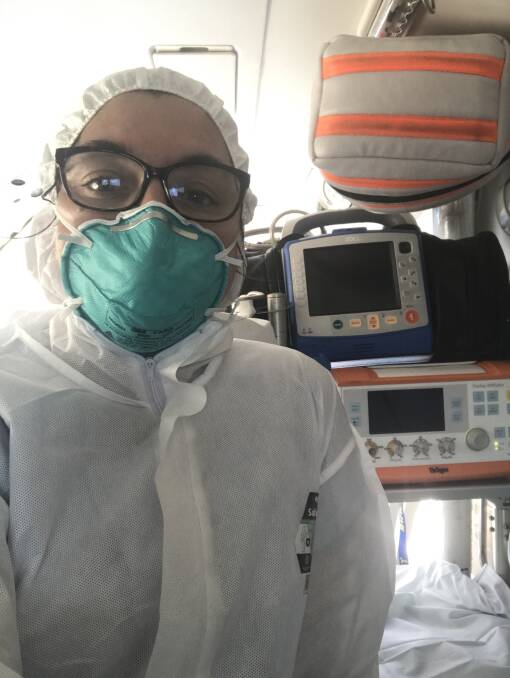
"We have a good work-life balance and we have been well-supported through this," Lydia says.
RFDS staff work four days on and then four days off.
Now with COVID alert transfers though one transfer that may have taken two hours before now turns into eight hours due to protocols and lengthy decontamination of everything including the inside of the plane.

But so far there have been no cases of COVID transferred in NSW by the RFDS.
But if any patient shows signs of a sore throat or a raised temperature it's immediately treated as a possible COVID, that means the flight goes into full protective mode.
There have been eight such transfers since the COVID alert started, and Lydia has done two of them.
None of the cases have ended up being positive to COVID-19, and it's a blessing for the bush it has remained COVID free for many months.
It's a laborious task having to protect the RFDS equipment, sanitise interiors, even at one stage having to wipe down each little crevice in the interior of the plane, until a cabin decontamination 'smoke bomb' was acquired.
But with the virus hitting a second wave in Victoria and some parts of NSW, it's not sure how long that COVID-free status for western NSW will last, especially with travellers heading north to Queensland on regional highways.
"I feel lucky and grateful that I do have the job that I do," Lydia says. "At least I'm secure and can provide the care that's needed at the time. This year will definitely be a year to remember and I believe it will make us stronger and more resilient."
It's a job where she rarely sees the outcomes of the patients but had had a couple of happy return transfers with patients she has seen before, one of them in remission after battling cancer.
Meantime, the pandemic has put pressure on the finances of the RFDS.
According to Dr Randall Greenberg, chief medical officer of the RFDS South-Eastern section, says it has lost funds through the temporary closure of RFDS visitor centres at Dubbo and Broken Hill, and donations have dried up mainly due to the ongoing economic pressures on the average persons' pocket.
Luckily the RFDS has sourced adequate PPE wear with a stockpile held in its Melbourne office that could see it through at least two months' supply.
The Federal Government has also stepped in with funds to help the RFDS source PPE and also get PPE to outlying health services.
The NSW Government and targeted private donations has also boosted PPE funds.
But Dr Greenberg says there has been a financial hit to the service. (It performs about eight transfers a month in NSW).
"We've lost a significant amount of income that we would normally get through charity drives," he said.
"Governments have stepped in but there's definitely been a shortfall." The RFDS also had to perform new tasks such as helping with COVID testing on the NSW-Victorian border.

"Even though there have been no COVID-19 cases in western NSW, any patient, even with shorter breath, we have to treat as a suspect COVID case," he said.
"So we have to don full gowns and goggles and follow all the proper procedures." Although this PPE wear was not too heavy, it would be a "terrible" imposition on RFDS staff come summer from sweating up in the heat.
Dr Greenberg has 35 years' experience as a doctor and works in hospitals.
If there was any good out of the COVID-19 alert, it was that infection controls had improved.
Having to deal with many diseases over the years, he didn't "fear" getting COVID, but was deeply concerned about the disease itself and had seen the great trauma it had inflicted on many areas of the world.
"Should I be scared? I don't think I am. My whole career has been working in hospitals where I could contract anything. You get an attitude that 'this is what I do'."


